When a vial fails, it is never “just packaging”. It is lost batches, stability worries, and regulatory headaches that nobody wants to explain.
You choose pharmaceutical glass bottles by matching Type I/II/III to your formulation, then locking in a compatible closure, sterilization route, and E&L strategy that you can scale from pilot to launch.

Once I see route of administration, pH, and process flow, the correct glass family and closure options usually narrow fast. After that, it becomes a negotiation between risk, cost, and lead time.
How do I choose between USP Type I, II, and III based on my formulation?
If you start from price instead of risk, you often end up re-doing studies later. The safest route is to start from route, pH, and hydrolytic resistance first.
For injectables and high-risk drugs, default to Type I; use Type II for less aggressive aqueous products; keep Type III for non-parenteral or solid forms, then confirm fit with pharmacopeial hydrolytic tests.

In practice, Type I, II, and III are not just names. Under USP <660> Containers—Glass 1 and Ph. Eur. 3.2.1 Glass containers for pharmaceutical use 2, they are performance classes defined by hydrolytic resistance and how much alkali the glass gives up to water. Type I glass usually has a borosilicate composition and the highest hydrolytic resistance by its bulk chemistry. Type II starts as soda-lime but gets a surface treatment (often sulfur based) that upgrades the inner surface resistance. Type III is untreated soda-lime glass with only moderate hydrolytic resistance.:contentReference[oaicite:0]{index=0}
For parenterals, biologics, and pH-sensitive drugs, Type I is my default. It covers most acid, neutral, and many alkaline injectables, and it tolerates autoclave cycles and lyophilization far better than other families. For acidic or neutral aqueous products that are less critical, including some parenterals and many oral liquids, Type II can be an option, but only after compatibility and stability studies confirm that the surface treatment holds up under your process and storage conditions. For non-aqueous, oral, and solid forms like tablets, capsules, and some syrups, Type III is usually acceptable. Many cough syrups and OTC liquids use Type III bottles without issues, because local pH and excipients do not aggressively attack the glass.:contentReference[oaicite:1]{index=1}
Color is the second lever. If your molecule fails ICH Q1B photostability testing 3, you may need amber or stronger light protection. I read the ICH Q1B data and ask a simple question: is amber Type I or II enough, or do we need extra cartons, sleeves, or labels to reach the required light resistance? Remember, ICH Q1B’s standard exposure (≈1.2 million lux-hours visible + 200 Wh/m² UVA) is harsh, but it reveals how much real protection you need from the primary container versus secondary packaging.:contentReference[oaicite:2]{index=2}
So first match route + pH + light sensitivity to a glass type and color. Only then start trading between Type I and Type II on cost, and always keep the pharmacopeial hydrolytic classification in your regulatory story.
How do I match closure systems and sterilization to my filling line?
A perfect vial with the wrong stopper system is still a failure. Container-closure integrity and process compatibility matter as much as the glass itself.
Pick vial neck, stopper, and seal as one system that fits your filling machine, sterilization method, and CCIT strategy, instead of treating them as separate purchases.
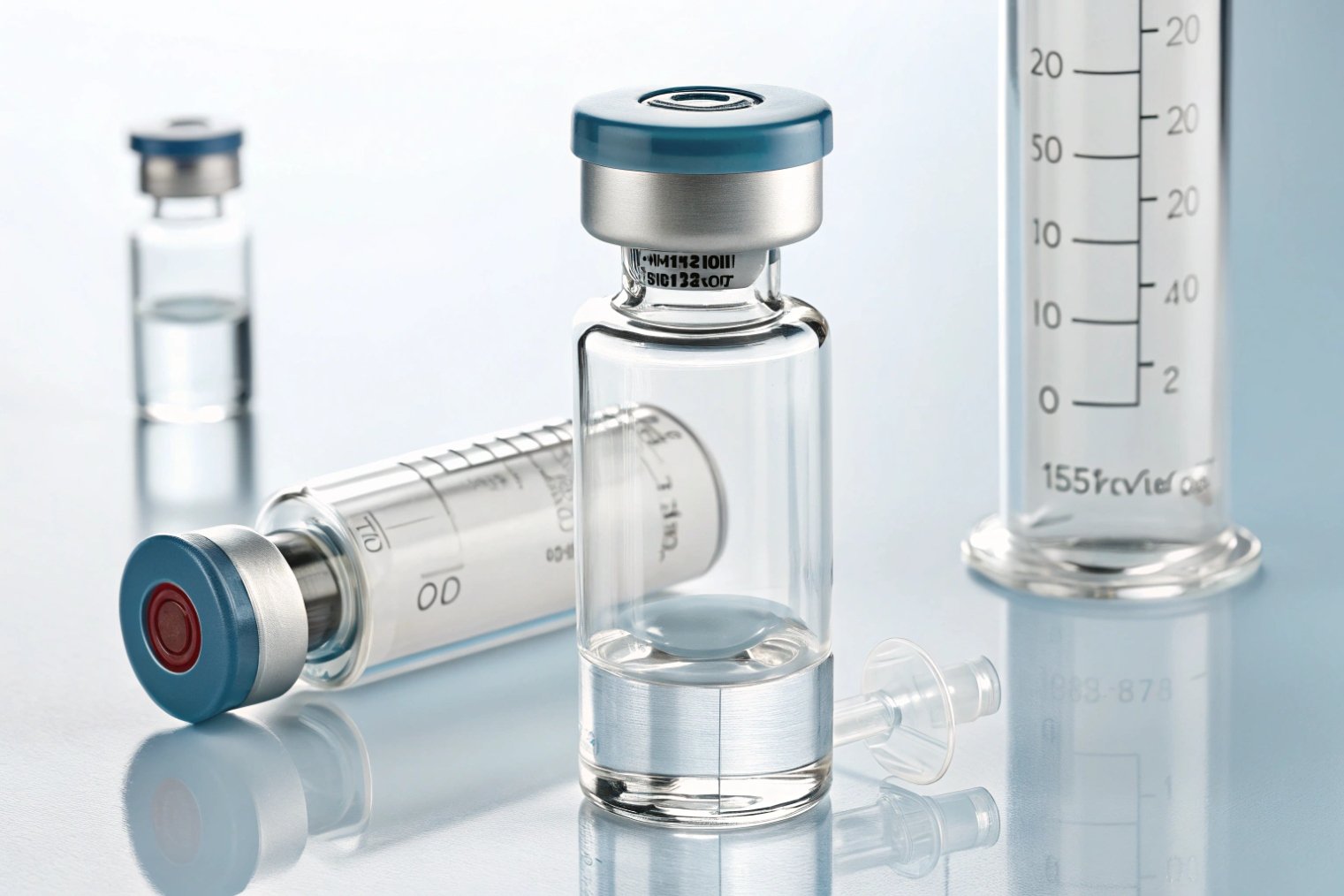
The starting point is your vial format. Tubular vials (from glass tubing) have tight dimensional tolerances and thin bases, which is ideal for lyophilization and many SVIs (small volume injectables). Molded vials and bottles have thicker walls and bases, more mechanical robustness, and suit LVIs or oral syrups better. Whatever format you choose should fit standard neck finishes (for example ISO 8362 dimensions for injectable vials 4), because that locks you into a wide range of compatible stoppers and aluminum seals.:contentReference[oaicite:3]{index=3}
Next, line up closure and elastomer. For injectables you usually choose a rubber stopper (bromobutyl, chlorobutyl, or advanced formulations), sometimes with fluoropolymer coatings to reduce extractables and sticking. Flip-off or plain aluminum seals complete the system. Here I think in terms of container-closure integrity (CCI): Will this stopper and crimp profile hold vacuum or pressure through shipping, freeze-thaw, autoclave, and long storage? Modern guidance like USP <1207> Container Closure Integrity 5 pushes you toward deterministic CCI methods (helium leak, vacuum decay, headspace gas analysis) instead of only dye ingress. It makes sense to choose components that are already validated in those methods by either you or the closure supplier.:contentReference[oaicite:4]{index=4}
Sterilization then filters your options. If you plan to steam sterilize filled vials (terminal moist-heat), both glass and closure must tolerate the autoclave cycle with no delamination, stopper shrinkage, or seal deformation. If you sterilize components separately (vials in depyro tunnel, stoppers in autoclave, seals gamma or EtO) and use aseptic filling, you must ensure all materials keep their functional properties after that pre-treatment. Many teams now move to RTU (ready-to-use) nests and tubs, where vials and syringes arrive pre-washed and pre-sterilized; those formats come with stricter dimensional and surface specs, but they save time on the filling line.
For oral or OTC medicines, you may also need child-resistant, senior-friendly, and tamper-evident closures that meet national rules (for example US PPPA under 16 CFR Part 1700 6). That instantly shapes bottle neck selection and liner choice, because not every glass finish has a matching CR cap. In all cases, I treat vial + closure + sterilization as one design problem, not three separate orders.
How do I evaluate extractables, leachables, and hydrolytic resistance?
Choosing “Type I” on paper is not the end of the story. Real formulations can still drive ion exchange, delamination, or unexpected leachables.
Use pharmacopeial hydrolytic tests to qualify glass type, then build a risk-based extractables and leachables program (including USP <1660> surface durability studies) to see how your real drug product stresses that glass over time.

Hydrolytic resistance is the first gate. USP <660> and Ph. Eur. 3.2.1 describe tests that measure how much alkali dissolves into purified water after controlled autoclave conditions. Results line up with Type I, II, or III classification. Under the revised USP <660>, these types are defined by performance, not just composition, so some newer high-durability glasses can still qualify as Type I even if they are not classic borosilicate formulas.:contentReference[oaicite:5]{index=5}
But hydrolytic class alone does not tell you whether your specific formulation will be safe. Buffers, chelators, surfactants, and pH can all accelerate attack on the inner surface. That is where extractables and leachables (E&L) work comes in. I like to start with vendor extractables data on their glass and closures, then design targeted leachables studies using your real formulation under ICH storage conditions. These studies usually combine ICP-MS for metals, LC/GC-MS for organics, and targeted methods for known risk species.
For glass itself, USP <1660> Evaluation of the Inner Surface Durability of Glass Containers 7 is the key chapter on inner surface durability and delamination risk. It explains how to screen vials under stressed conditions (higher temperature, aggressive formulations) and how to compare different glass lots or suppliers. The goal is to detect early signs of flaking or lamella formation before you commit to a container on which your product may sit for years. Many labs now use USP <1660> as a framework to rank vials and to justify switching to higher-durability compositions or coatings when delamination risk is high.:contentReference[oaicite:6]{index=6}
Light sensitivity is the last layer. ICH Q1B photostability tests tell you whether your active or finished product degrades under standard light exposure. If it does, you must decide how much protection the primary glass gives (amber or other light-resistant types) and how much must come from secondary packaging. I often see teams save cost by using clear Type I with very strong outer cartons, but only when photostability data clearly supports that choice.:contentReference[oaicite:7]{index=7}
So the flow is simple: confirm hydrolytic class, study extractables and leachables, evaluate inner surface durability with a USP <1660> style program, and overlay photostability results. Together they tell you if this bottle is a quiet partner for the drug or a long-term risk.
What MOQs and lead times make sense for pilot versus scale-up?
Even the perfect technical choice fails if you cannot get it on time. For glass, supply, MOQ, and lead time shift a lot between early development and commercial scale.
Use low-volume standard vials and bottles for development and early clinical work, then lock your commercial design early enough that mold investment, MOQ, and lead time do not block your launch.

During pre-formulation and Phase I/II, flexibility is more important than unit price. I normally suggest:
- Standard ISO tubular vials in Type I (both clear and amber) that many suppliers stock.
- MOQs in the range of a few thousand to one or two full pallets, depending on format.
- Off-the-shelf stoppers and seals, even if they are not the final brand look.
This lets you run small batches, change fill volumes, and tweak processes without getting stuck with large obsolete glass inventory. Lead times here can be weeks rather than months, especially if you use a distributor that already holds stock.
As you move into Phase III and process validation, you should converge on the commercial container-closure system. At this point, MOQs start to move up, especially for:
- Custom molded bottles or larger infusion containers.
- Special colors or glass types that need dedicated furnace campaigns.
- Embossed logos or unique neck finishes.
For molded pharma bottles, practical MOQs often start around 50,000–100,000 pcs per run for a custom design, sometimes more. For standard tubular vials, you can still buy in smaller lots, but you may want supplier contracts that cover the first several commercial years to protect capacity. Color changes and new molds also add weeks or months to the first delivery, so I like to align mold sign-off well before pivotal stability lots.
Lead time planning differs by scale:
- Pilot and clinical: plan for 4–8 weeks for standard vials and closures, longer only if import approvals or special sterilization are needed.
- Commercial: plan for several months for custom molded or large-volume Type I bottles, especially if you need RTU formats, special surface treatments, or alignment with new production lines.
For our own glass projects, the smoothest launches happen when the team treats packaging as part of the formulation, not as a last-minute purchase. If you align Type selection, closure, E&L strategy, and MOQ planning early, glass stops being a constraint and becomes a stable platform that follows the product from the first vial into patients all the way to global commercial scale.
Conclusion
Choosing pharma glass is about risk and reliability: match the right Type and closure to your drug early, then scale only when glass, line, and data already agree.
Footnotes
-
Official USP chapter reference for glass container classification and testing expectations. ↩ ↩
-
Entry point for European Pharmacopoeia requirements used in EU-facing regulatory strategies. ↩ ↩
-
Helps verify whether primary packaging must be light-resistant or supported by secondary cartons. ↩ ↩
-
Confirms standardized vial dimensions that drive stopper, seal, and crimp compatibility. ↩ ↩
-
Practical framework for selecting and validating deterministic container-closure integrity test methods. ↩ ↩
-
U.S. regulatory basis for child-resistant packaging requirements that affect neck and closure selection. ↩ ↩
-
Screening approach for inner-surface durability and delamination risk under stressed storage. ↩ ↩








